H Pylori
All the information provided here including recommendations and suggestions should be treated for informational purposes only and not a coercion to follow.
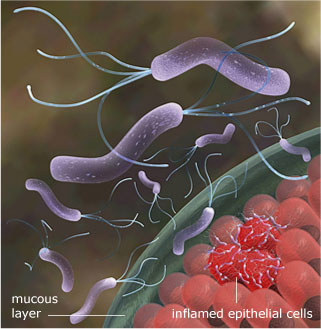
It is one of the most common infections worldwide and the indications for treatment and eradication are:
Grade A:
Peptic ulcer disease
MALToma
Patients’ wishes (after full consultation with their physician)
Non-ulcer dyspepsia
To reduce the risk of peptic ulcer and upper gastrointestinal bleeding in non-steroidal anti-inflammatory drug-naive users
As a strategy for gastric cancer prevention in communities with high incidence of gastric cancer
Grade B:
Atrophic gastritis
After gastric cancer resection
Patients who have first degree relatives of patients with gastric cancer
Before starting long-term aspirin therapy for patients at high risk for ulcers and ulcer-related complications
Patients receiving long-term low-dose aspirin therapy and who have a past history of upper gastrointestinal bleeding and perforation
Gastroesophageal reflux disease patients requiring long-term proton pump inhibitor
Grade C:
Unexplained iron-deficiency anemia, or idiopathic thrombocytopenic purpura
Even though the prevalence of HPylori is decreasing, its diagnosis should still be at the forefront of possible diagnosis.
Points of interest:
- If there is no alarm symptoms, test and treat is an acceptable strategy uninvestigated dyspepsia
- Test and treat is no longer recommended for GERD unless plan to receive long term PPI
- Testing is recommended for communities with high incidence of gastric cancer
- H Pylori eradication will reduce the risk of PUD and GIB in NSAID naïve subgroup but it alone is inadequate in the subgroup of long term NSAID users where they have past h/o PUD or PUD complications
- If the patient has high risk of PUD and starting on long term ASA, they should be tested and treated for HP even though eradication alone is inadequate.
- As a last resort, HP should be tested for in unexplained IDA and ITP
- UBT and stool antigen test are accurate and appropriate for confirmation of H Pylori while serological test has very limited role
Possible treatment regimes for HP
A) If no penicillin allergy:
First line: PPI + Amoxycillin + Clarithromycin bd for 7 days
Second line: Rabeprazole + Amoxycillin + Clarithromycin bd for 14 days
OR Rabeprazole + Amoxycillin + Metronidazole bd for 14 days
Third line: PPI + Levofloxacin + Amoxycillin for 10 days
Fourth step: need to consider Rifabutin or Bismuth or send for C&S
B) If penicillin allergy:
PPI + Metronidazole + Clarithromycin bd for 7 days
C) Sequential therapy:
First 5 days: PPI + Amoxycillin bd
Next 5 days: Clarithromycin and Tinidazole bd
edited 12th July 2010